 Herman AesthÉtiques
Herman AesthÉtiques
Breast Lift (Mastopexy)
Lift. Rebalance. Refine.
A mastopexy restores a higher, firmer breast contour by correcting breast ptosis, tightening the cutaneous envelope, and repositioning the nipple–areola complex (NAC) on a vascularized pedicle.
Overview
What a Lift Corrects
Ptosis occurs when the breast parenchyma descends and the NAC sits at or below the inframammary fold (IMF). During mastopexy, redundant skin is excised, the parenchyma is coned and re-suspended, and the IMF relationship is refined to restore base support and upper-pole projection.
Technique choice is guided by ptosis grade, skin quality, areolar diameter, breast base width, and desired scar vector.
Technique Options
Lift Patterns
Incision design and pedicle selection are tailored to ptosis grade and tissue biomechanics.
A circumareolar (“donut”) mastopexy for mild ptosis. Also allows areolar reduction with limited scar length.
Best when the NAC is only slightly below ideal position and skin redundancy is minimal.

Periareolar + vertical limb (“lollipop”) for moderate ptosis. Enables stronger parenchymal coning and improved projection.
Common pedicles include superomedial or superior to preserve perfusion.
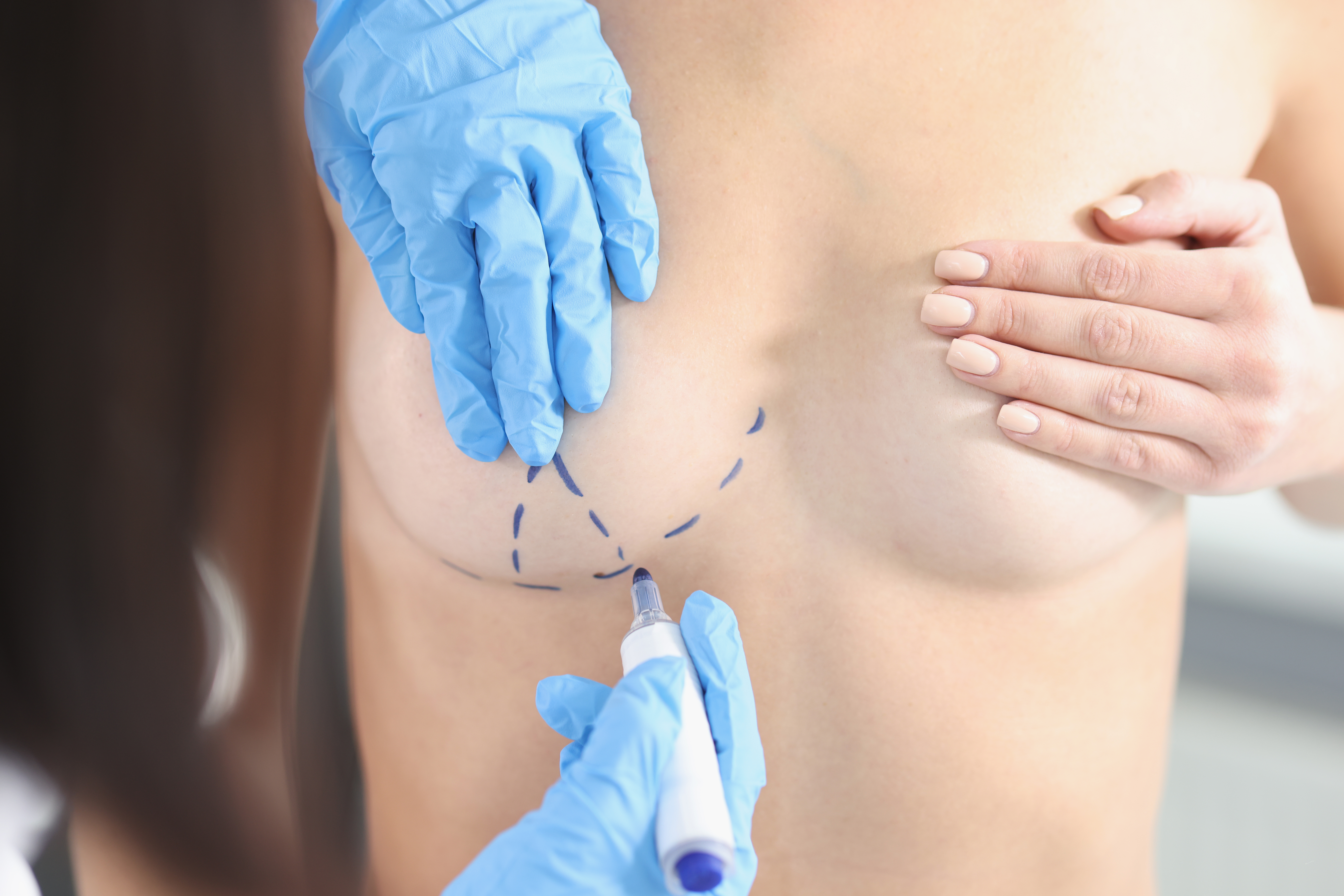
Adds a horizontal IMF limb (“anchor”) for significant ptosis or marked dermatolaxia. Greatest ability to excise excess skin vectors.
Useful when the lower pole requires extensive tightening to prevent bottoming out.
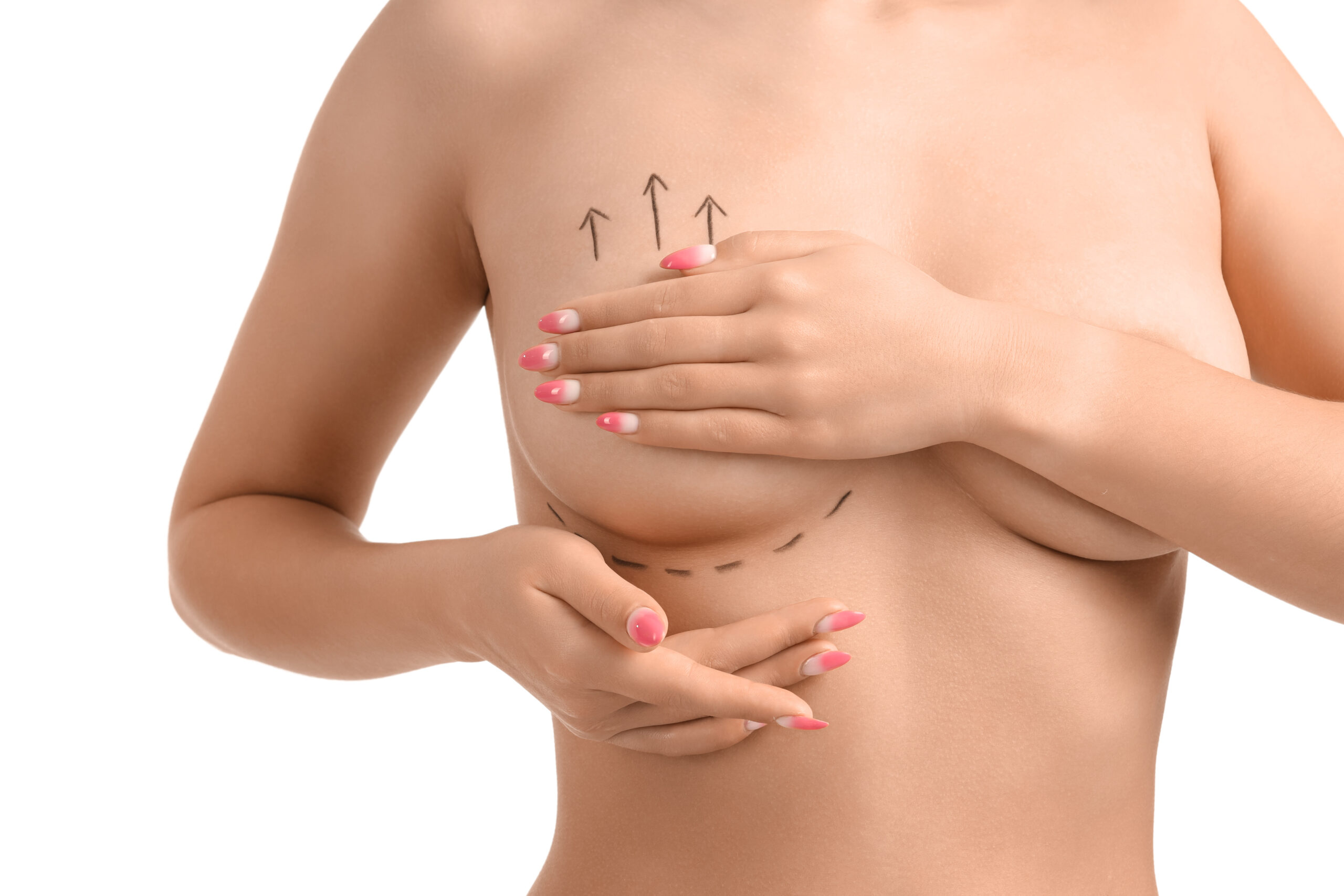
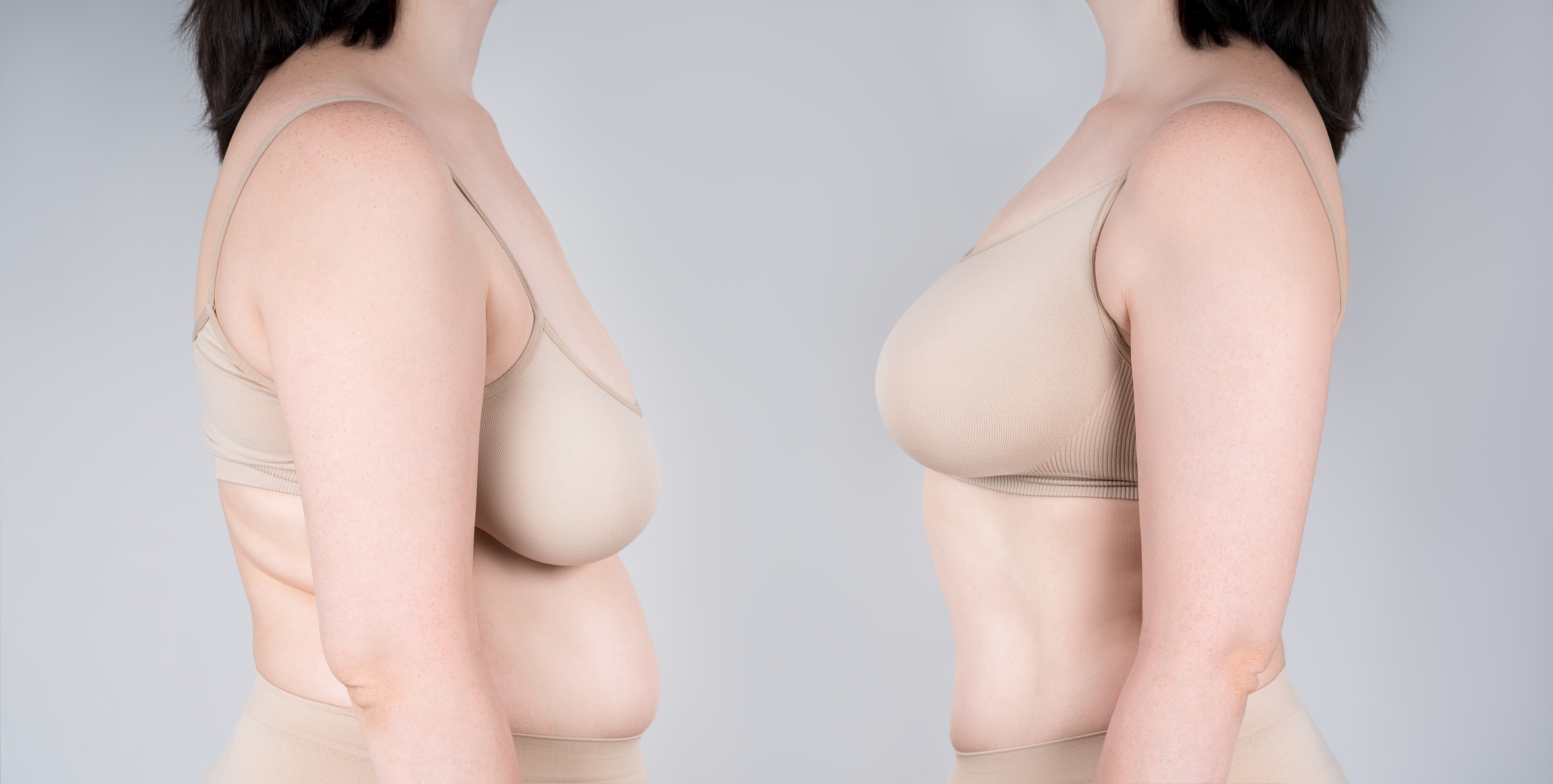
Augmentation mastopexy combines lift + implant when volume loss (postpartum involution) accompanies ptosis.
Implant selection considers base width, tissue pinch thickness, and desired projection to avoid over-stretching.
Terminology
Key Medical Terms
Tissue stalk preserving NAC neurovascular supply during transposition.
Severity classification based on NAC position vs IMF and mound apex.
Glandular + fatty tissue reshaped into a higher, tighter cone.
Excess lax skin envelope requiring excisional tightening.
Superior rotation of your own tissue to improve upper-pole fullness.
Healing
Recovery Phases
Swelling (edema) and tightness are expected early. Shape refines as the parenchyma settles into its new support.
Week 1
Compression bra, light ambulation, avoid heavy lifting. Watch for hematoma or seroma.
Weeks 2–3
Edema decreases. NAC position stabilizes. Gentle range-of-motion resumes.
Weeks 4–8+
Return to full exercise when cleared. Scars transition into remodeling over 6–12 months.
Safety First
Risks & Monitoring
Complications are uncommon but clinically important to understand.
Additional considerations include infection, asymmetry, altered sensation, and the need for revision.
Questions, Answered
Breast Lift FAQ
Does mastopexy increase breast size?
How is the scar pattern chosen?
Can a lift be combined with reduction?
How long do results last?
Schedule Your Consultation
Meet with Dr. Herman to review ptosis grading, pedicle options, and the lift technique best suited to your anatomy and goals.
Book NowBreast Aesthetic Expertise
Why Choose
Dr. Herman
Dr. Herman balances refined elevation with surgical safety — emphasizing pedicle perfusion, symmetry, and durable parenchymal support.
- Advanced training in aesthetic & reconstructive breast surgery
- Technique tailored to ptosis grade and tissue biomechanics
- Scar-vector planning for stable, long-term contour

Patient Testimonials
Real stories. Real results.
“I have been going to this office for years and wouldn’t go anywhere else. The treatment is consistently excellent and I always feel cared for.”
Read full review →“This man is not only an excellent surgeon — he is an artist. He changed my life and gave me confidence I never had. His work is stellar and his staff is amazing.”
— Stefanie F. (Plastic Surgery Near You)
Read full review →“Dr. Herman corrected a nose job I had 10 years ago. He did exactly what I asked for and I love my results — even with swelling. The entire experience was relaxing and comfortable.”
— Ondraia R. (Plastic Surgery Near You)
Read full review →“I finally feel comfortable in my own body. His calm and steady approach made all the difference.”
Read full review →“The staff was warm, welcoming, and knowledgeable. Dr. Herman is brilliant. I travel from New York because he is the only one I trust.”
— Verified Patient Review (Feb 27 2025)
Read full review →“Dr. Herman and his staff are exceptional. Caring, thorough, and truly invested in your well-being. I wouldn’t go anywhere else.”
— Verified Patient Review (Jul 15 2025)
Read full review →“Dr. Herman is THE BEST physician I have ever had. His bedside manner is the best. He is easy to talk to and has a great sense of humor. He truly cares about his patients, and his office staff was so welcoming and accommodating. My only regret is that I didn’t go to him sooner.”
— Verified Patient Review (Jul 1, 2022)
Read full review →“My wife had a cyst removed from her back. Dr. Herman was personable and professional. Minor surgery was done in the office and we were out in about 30 minutes. Staff was considerate and caring. I’m sure we would use Dr. Herman for any future plastic surgery needs.”
— Freddy A. (Plastic Surgery Near You)
Read full review →“Dr. Herman is absolutely the best! He is knowledgeable and professional. He has changed my life forever and made my dream come true. I am very, very pleased with the results! Thank you Dr. H!!!”
— Nicola G. (Plastic Surgery Near You)
Read full review →“Dr. Herman is a great surgeon — very trustworthy. I highly recommended.”
— Evelyn I. (Plastic Surgery Near You)
Read full review →“Dr. Herman & his staff are one of the best I have experienced. They are caring & know how to deal with their patients. I couldn’t have asked for a better group of physicians.”
— Verified Patient Review (Sep 4, 2025)
Read full review →“This is my second procedure with Dr. Herman. He is amazing. Caring and thorough. Professional. Highly skilled. Would highly recommend him and his practice.”
— Verified Patient Review (Jun 10, 2025)
Read full review →“I have gone to Dr. Herman’s office for years. Everyone there is more like family, and they treat you with the utmost care. I would send everyone there to them.”
— Verified Patient Review (Apr 24, 2025)
Read full review →“Appointment was on time, all my questions were answered. Staff and doctor were very knowledgeable and pleasant. Got fast results — I’m glad I chose this office.”
— Verified Patient Review (Apr 29, 2025)
Read full review →“Wonderful Dr. and PA. Knowledgeable and efficient while being caring and supportive.”
— Verified Patient Review (Apr 24, 2025)
Read full review →“My medical care was outstanding. Dr. Herman is the consummate professional. I want to thank his staff as each member was very kind and thoughtful.”
— Verified Patient Review (Apr 17, 2025)
Read full review →“I am thrilled with the way I’m treated as a patient of Dr. Herman’s. Everyone is always polite and kind — I’m really grateful.”
— Verified Patient Review (Mar 27, 2025)
Read full review →“Excellent — professional, friendly, and efficient. Demonstrated extra care to ensure my understanding of the procedure. Comforting.”
— Verified Patient Review (Mar 25, 2025)
Read full review →“Great thorough experience. Extremely pleased with all staff.”
— Verified Patient Review (Mar 4, 2025)
Read full review →“Dr. Herman is a fantastic doctor. His office is very accommodating to get me in. I completely trust him with my care.”
— Verified Patient Review (Jan 28, 2025)
Read full review →“Dr. Herman and his staff are marvelous. They are a 10. They are wonderful.”
— Verified Patient Review (Mar 20, 2025)
Read full review →“The office staff is always so welcoming and make me feel very comfortable. Dr. Herman is professional, calms me down, and I completely trust him. I would never go anywhere else.”
— Verified Patient Review (Jul 15, 2025)
Read full review →“Dr. Herman is one of the finest providers I have ever dealt with. He handled my problem with confidence and quickness. His expertise is otherworldly.”
— Verified Patient Review (Dec 3, 2024)
Read full review →“Dr. Herman is an exceptional physician. I greatly value his care and appreciate his expertise. He is extremely compassionate and personable.”
— Verified Patient Review (Oct 17, 2024)
Read full review →“Dr. Herman and his staff made me feel very comfortable. They are professional and ‘down to earth.’ I would never go anywhere else for the services I require.”
— Verified Patient Review (Sep 12, 2024)
Read full review →“Dr. Herman is excellent in communication, knowledge, and surgical skills. I trust him totally!”
— Verified Patient Review (Aug 6, 2024)
Read full review →“The visit was perfect — from the doctor to the staff to the cleanliness of the office. Everything was great. Thank you so much.”
— Verified Patient Review (Jun 27, 2024)
Read full review →“Great experience. Staff was polite and helpful. Dr. Herman was professional and caring, explained what he was going to do, performed it masterfully, and arranged follow-up care.”
— Verified Patient Review (May 16, 2024)
Read full review →“Dr. Herman and his staff are extremely professional and supportive. My concerns were addressed by the entire team — I’m so happy I was referred here!”
— Verified Patient Review (Feb 15, 2024)
Read full review →“Dr. Herman and his staff are amazing. He really cares for his patients, shows concern and compassion, and will not cut corners. Probably the best LVHN has to offer.”
— Verified Patient Review (Jan 9, 2024)
Read full review →“I have the utmost respect for Dr. Herman and complete confidence in him. I’ve been going to this office for many years — his staff are wonderful too.”
— Verified Patient Review (Oct 3, 2024)
Read full review →“Dr. Herman & his staff treated me with respect and kindness. He took great care of me throughout the whole process — truly grateful.”
— Verified Patient Review (Jul 10, 2025)
Read full review →“Staff is fantastic — answered all of my questions and did a great job alleviating concerns.”
— Verified Patient Review (Jun 12, 2025)
Read full review →“Dr. Herman is an amazing practitioner. His ability exceeds others. He’s also personable — his people skills match his genius as a plastic surgeon.”
— Verified Patient Review (May 21, 2024)
Read full review →“One of the most friendly offices I have ever been to. Wonderful staff, and the doctor took his time, explained everything, and addressed my concerns.”
— Verified Patient Review (May 9, 2024)
Read full review →“Very professional service and care, polite, and made the experience as good as possible. The A team.”
— Verified Patient Review (Apr 3, 2025)
Read full review →“He’s a wonderful, wonderful doctor. I’m so glad that I found him.”
— Verified Patient Review (Sep 24, 2024)
Read full review →“I couldn’t be more pleased with the exceptional care I receive at this office. A+ in every way.”
— Verified Patient Review (Jan 25, 2024)
Read full review →“Dr. Herman is an excellent doctor. His staff is courteous, polite, and knowledgeable. He explains everything thoroughly so you understand, and always answers questions.”
— Verified Patient Review (Jul 2, 2024)
Read full review →“Great experience from beginning to end.”
— Verified Patient Review (May 22, 2025)
Read full review →“Dr. Herman is very thorough and informative. He is courteous and concerned about your health. I am very grateful to have been sent to him — his staff is also excellent.”
— Verified Patient Review (Dec 10, 2024)
Read full review →“Always treated well. I’ve experienced being treated differently as I get older, but not at this practice. I appreciate that so much.”
— Verified Patient Review (Dec 19, 2024)
Read full review →“Caring, highly competent — wonderful feedback from everyone I have spoken to. He is definitely an asset to the hospital.”
— Verified Patient Review (Jan 28, 2025)
Read full review →“Everyone was very nice & understanding when I arrived a bit late. Dr. Herman was extremely pleasant in answering all my questions. I am hopeful for a great outcome.”
— Verified Patient Review (Feb 11, 2025)
Read full review →“I always feel confident with Dr. Herman as my care provider. He explains everything and is up to date with products that are best for me.”
— Verified Patient Review (Feb 13, 2025)
Read full review →“Dr. Herman has been seeing me for 3 years. He has been diligent in trying to resolve the issue.”
— Verified Patient Review (Apr 3, 2025)
Read full review →“Dr. Herman explained everything very well and answered all of my questions. His PA was also exceptional — kind, friendly, and gave great instructions.”
— Verified Patient Review (Nov 5, 2024)
Read full review →“They listened and took action when I was very concerned, hoping for a sooner resolution. I’m grateful.”
— Verified Patient Review (Oct 10, 2024)
Read full review →“Dr. Herman and his staff were amazing. I arrived early while they were on lunch, and they still welcomed me in. He explained everything in a way I understood. I’m very pleased with the service I received.”
— Verified Patient Review (Mar 20, 2025)
Read full review →“I love the professionalism of the office and Dr. Herman is awesome. I would recommend him to anybody.”
— Verified Patient Review (Apr 10, 2025)
Read full review →“Dr. Herman is the absolute best!!! I will always choose him.”
— Verified Patient Review (Nov 21, 2024)
Read full review →“Dr. Herman listened to my concerns and gave me answers.”
— Verified Patient Review (Oct 15, 2024)
Read full review →“Dr. Herman is one of the kindest and caring doctors I have ever known. I am very confident in his medical abilities.”
— Verified Patient Review (Oct 3, 2024)
Read full review →“I’ve seen Dr. Herman numerous times for different health issues. He’s the best, and so is his staff!”
— Verified Patient Review (Jun 18, 2024)
Read full review →“This office is amazingly wonderful, kind, and welcoming. Very knowledgeable — when you walk in the door, you feel at ease.”
— Verified Patient Review (Jul 16, 2024)
Read full review →“The provider was excellent — I felt comfortable knowing I was in his care. From check-in to check-out, I was treated excellently!”
— Verified Patient Review (Jul 30, 2024)
Read full review →“I am currently pleased and satisfied with Dr. Herman. He looked out for my well-being, made sure I addressed other health issues first, and never made me feel like it was about money. That showed me great care.”
— Verified Patient Review (Aug 28, 2025)
Read full review →“Good experience and I’ll be happy to continue treatment with Dr. Herman.”
— Verified Patient Review (Jul 24, 2025)
Read full review →“Dr. Herman serviced me really well and made sure I had all the testing done properly. He explained next steps clearly, so overall the experience was excellent.”
— Verified Patient Review (Jun 12, 2025)
Read full review →“I received exceptional care and an exceptional experience.”
— Verified Patient Review (Jun 25, 2024)
Read full review →“I believe Dr. Herman has the knowledge and expertise to deal with my problem.”
— Verified Patient Review (Jun 4, 2024)
Read full review →“Dr. Herman and PA are great. Highly recommend to all of my friends.”
— Verified Patient Review (Jan 30, 2024)
Read full review →“Excellent experience, knowledge, and care.”
— Verified Patient Review (Feb 20, 2025)
Read full review →“Doctor is wonderful, wonderful, wonderful. He acknowledges you, asks questions, and is just an amazing doctor.”
— Verified Patient Review (Feb 11, 2025)
Read full review →“Consolation for surgery. Herman and his staff are awesome.”
— Verified Patient Review (Feb 4, 2025)
Read full review →“I have been pleased with all of my procedures I’ve had with Dr. Herman and will continue to see him in the near future.”
— Verified Patient Review (Jan 16, 2025)
Read full review →“Dr. Herman is an exemplary physician and I wish more were like him.”
— Verified Patient Review (Jan 28, 2025)
Read full review →“Dr. Herman is a very conscious and very caring doctor. Very worried about your well-being and answered all of my questions.”
— Verified Patient Review (Apr 29, 2025)
Read full review →“The staff was warm, welcoming, and knowledgeable. Dr. Herman is brilliant — a gifted surgeon and kind human being.”
— Verified Patient Review (Feb 27, 2025)
Read full review →“Very caring — tried drops before jumping into surgery. Staff very helpful and polite.”
— Verified Patient Review (Jun 27, 2024)
Read full review →“Dr. Herman is a fantastic doctor. I completely trust him with my care and wouldn’t consider any other doctor for my needs.”
— Verified Patient Review (Jan 28, 2025)
Read full review →“Dr. Herman and his staff are wonderful people. I couldn’t ask for a better doctor and staff.”
— Verified Patient Review (Oct 8, 2024)
Read full review →“Overall made me feel comfortable with my issue.”
— Verified Patient Review (Jul 18, 2024)
Read full review →“They are fast and on point with the professional.”
— Verified Patient Review (Jul 15, 2025)
Read full review →“Excellent experience, knowledge and care.”
— Verified Patient Review (Feb 20, 2025)
Read full review →“Dr. Herman and the PA are kind and professional practitioners. They took care of my issue immediately, asked about my well-being, and showed compassion throughout. I have complete trust in their advice.”
— Verified Patient Review (Nov 21, 2024)
Read full review →“Dr. Herman is a very knowledgeable, kind, and courteous doctor. His staff is kind and helpful. He listens, gives advice, and helps you reach your goals.”
— Verified Patient Review (Nov 7, 2024)
Read full review →“I extend my satisfaction with my doctor, Dr. Herman. He is a top-notch, top-line doctor in my book. I commend him.”
— Verified Patient Review (Nov 7, 2024)
Read full review →“I have referred numerous people to Dr. Herman. He is wonderful, as well as his staff.”
— Verified Patient Review (Oct 29, 2024)
Read full review →“I felt that Doctor Herman was right on the mark.”
— Verified Patient Review (May 1, 2025)
Read full review →“This will be my 2nd surgery with Dr. Herman! He’s a quality physician!”
— Verified Patient Review (Sep 10, 2024)
Read full review →“Dr. Herman is a very good doctor, and his staff was very nice too.”
— Verified Patient Review (Aug 27, 2024)
Read full review →“Dr. Herman is a great doctor, very trustworthy. I highly recommend.”
— Evelyn Inoa Art (Plastic Surgery Near You)
Read full review →“Dr. Herman is amazing. Caring, thorough, professional, and highly skilled. Would highly recommend him and his practice.”
— Verified Patient Review (Jun 10, 2025)
Read full review →“Good experience and I’ll be happy to continue treatment with Dr. Herman.”
— Verified Patient Review (Jul 24, 2025)
Read full review →“Everyone was very nice & understanding. Dr. Herman was extremely pleasant and answered all my questions.”
— Verified Patient Review (Feb 11, 2025)
Read full review →“Dr. Herman is an amazing provider. He listens and is a skilled doctor.”
— Verified Patient Review (May 9, 2024)
Read full review →“Great experience, staff was polite and helpful. Dr. Herman was professional and caring.”
— Verified Patient Review (May 16, 2024)
Read full review →“I’m thrilled with the way I’m treated as a patient. Everyone is polite and kind. I’m really grateful.”
— Verified Patient Review (Mar 27, 2025)
Read full review →“Staff was warm, welcoming, and knowledgeable. Dr. Herman is brilliant… a true gift to the medical profession.”
— Verified Patient Review (Feb 27, 2025)
Read full review →“Dr. Herman is exceptional. Compassionate, personable, and thorough — the whole practice is outstanding.”
— Verified Patient Review (Oct 17, 2024)
Read full review →“I have been going to this office for years and wouldn’t go anywhere else. The treatment is consistently excellent, and I always feel cared for.”
Read full review →“Dr. Herman is THE BEST physician I have ever had. His bedside manner is the best. He is easy to talk to and has a great sense of humor. He truly cares about his patients and is kind, compassionate, and thoughtful. The entire office staff was welcoming, accommodating, and amazing. My only regret is not finding him sooner.”
Read full review →“This man is not only an excellent surgeon — he is an artist. He changed my life and gave me confidence I never knew I had. His work is stellar, and I will continue to go to him for future procedures. His support staff is amazing and professional.”
— Stefanie Franklyn (Plastic Surgery Near You)
Read full review →“AMAZING WORK! Dr. Herman corrected a nose job I had 10 years ago. He did exactly what I asked for — I love it, even with swelling. Dr. Herman and Amy made me feel so comfortable and relaxed. I recommend him to anyone considering plastic surgery.”
— Ondraia Robinson (Plastic Surgery Near You)
Read full review →“My wife had a cyst removed from her back. Dr. Herman was personable and professional. The in-office surgery was quick, and his staff was considerate and caring. We would absolutely return for future needs.”
— Freddy Anthony (Plastic Surgery Near You)
Read full review →“Dr. Herman is absolutely the best. He is knowledgeable, professional, and truly gifted. He changed my life and made my dream come true. I am thrilled with my results — thank you Dr. H!”
— Nicola G (Plastic Surgery Near You)
Read full review →“Dr. Herman is a great surgeon — very trustworthy. I highly recommend him.”
— Evelyn Inoa Art (Plastic Surgery Near You)
Read full review →“This is an outstanding practice and Dr. Herman and his team are the best!!!”
— Verified Patient Review (May 13, 2025)
Read full review →“I did not need a prescription. Dr. Herman and his staff are marvelous. They are a 10. Give them all raises.”
— Verified Patient Review (Mar 20, 2025)
Read full review →“Dr. Herman is very compassionate and personable. I greatly value his care and appreciate his expertise.”
— Verified Patient Review (Oct 17, 2024)
Read full review →“Dr. Herman is a very good doctor. His staff was very nice too — I felt comfortable the entire visit.”
— Verified Patient Review (Aug 27, 2024)
Read full review →“The staff was always so welcoming and accommodating. Everyone made me feel at ease from start to finish.”
— Verified Patient Review (Jul 16, 2024)
Read full review →“Dr. Herman is diligent and truly invested in resolving the issue. I’ve seen him for years and trust him completely.”
— Verified Patient Review (Apr 3, 2025)
Read full review →“Everyone there treats you with the utmost care. I’m so glad Dr. Herman is still in practice.”
— Verified Patient Review (Apr 24, 2025)
Read full review →“Dr. Herman is excellent in communication and surgical skills. I always feel confident in his care.”
— Verified Patient Review (Aug 6, 2024)
Read full review →